Preventing diabetes, a condition that's steadily on the rise, is no small feat. But it's crucial to know that we're not powerless against this health crisis. In fact, with the right lifestyle changes, such as integrating regular exercise into our daily routine, we can significantly reduce our risk of developing this chronic disease.
Exercise isn't just about losing weight or building muscle – it plays a vital role in regulating blood sugar levels too. Regular physical activity encourages our bodies to use insulin more efficiently and helps control weight—two factors that are key in managing and preventing diabetes. If you're wondering how much exercise is needed for optimal benefits, we'll guide you through the process.
We've all heard it before: "An ounce of prevention is worth a pound of cure." And when it comes to diabetes, never has this statement been truer. We don't have to stand by idly waiting for a diagnosis; instead, let's take charge and start making these healthy changes today.
Understanding the Link Between Exercise and Diabetes Prevention
We've all heard it before - regular exercise is good for our health. But did you know that it's particularly beneficial for diabetes prevention? Indeed, numerous studies demonstrate a strong correlation between physical activity and a reduced risk of developing this chronic illness.
Exercise plays a vital role in maintaining normal blood sugar levels. When we engage in physical exertion, our body uses glucose as an energy source, effectively lowering our blood sugar. It also increases insulin sensitivity, meaning our bodies can use insulin more effectively to convert glucose into energy.
Let's consider some data to reinforce these points:
| Benefits of Exercise | Impact on Diabetes |
|---|---|
| Lowered Blood Sugar | Reduced Risk |
| Increased Insulin Sensitivity | Improved Glucose Utilization |
Engaging in regular exercise doesn't have to mean hitting the gym hard every day. In fact, moderate-intensity activities like brisk walking, swimming or even gardening can do wonders. The American Diabetic Association recommends at least 150 minutes of moderate-intensity aerobic activity per week. That's only about 20 minutes per day – something achievable for most us.
Though it might be challenging to get started with an exercise routine if you're not used to it, remember that every bit counts. Start small and gradually increase the intensity and duration as your fitness improves over time.
And don't forget about strength training either. Including resistance exercises such as lifting weights or doing yoga twice a week can significantly improve your muscle strength and overall metabolic health – both essential components of diabetes prevention.
The Best Types of Exercises to Prevent Diabetes
We're glad you've made it here, because we've got some important information to share with you. We know that managing diabetes can be a challenging task. But what if we told you there are ways to prevent this condition through exercise? That's right. Regular physical activity is one of the most effective methods in preventing diabetes.
Now, let's talk about which exercises are best for this purpose. First on our list is aerobic exercise. This includes activities like brisk walking, running, biking or swimming. These exercises get your heart pumping and help increase insulin sensitivity. What does that mean? Well, when your body is more sensitive to insulin, it uses glucose from your bloodstream more effectively which helps keep blood sugar levels in check.
Next up: resistance training. Did you know that muscle tissue burns more calories than fat tissue even while at rest? So building muscle mass can boost metabolism and improve blood sugar control - making resistance training an excellent choice for diabetes prevention.
- Aerobic Exercises
- Brisk walking
- Running
- Biking
- Swimming
- Resistance Training
- Weight lifting
- Bodyweight exercises (like push-ups or squats)
But don't overlook the importance of flexibility and balance exercises either. Yoga and Tai Chi not only improve these aspects but also reduce stress levels—another crucial factor in managing and preventing diabetes.
So how much should you exercise? According to the American Diabetes Association, adults should aim for a minimum of 150 minutes of moderate-to-vigorous intensity aerobic activity per week along with two sessions of strength training.
All things considered though, any type of physical activity can contribute positively towards preventing diabetes. Just remember – start slow if needed and gradually build up the intensity as your fitness level improves. Exercise should be fun too. Choose activities that engage you both physically and mentally so it doesn't feel like a chore. With the right mindset and determination, we can all work towards a healthier lifestyle and prevent diabetes through exercise.
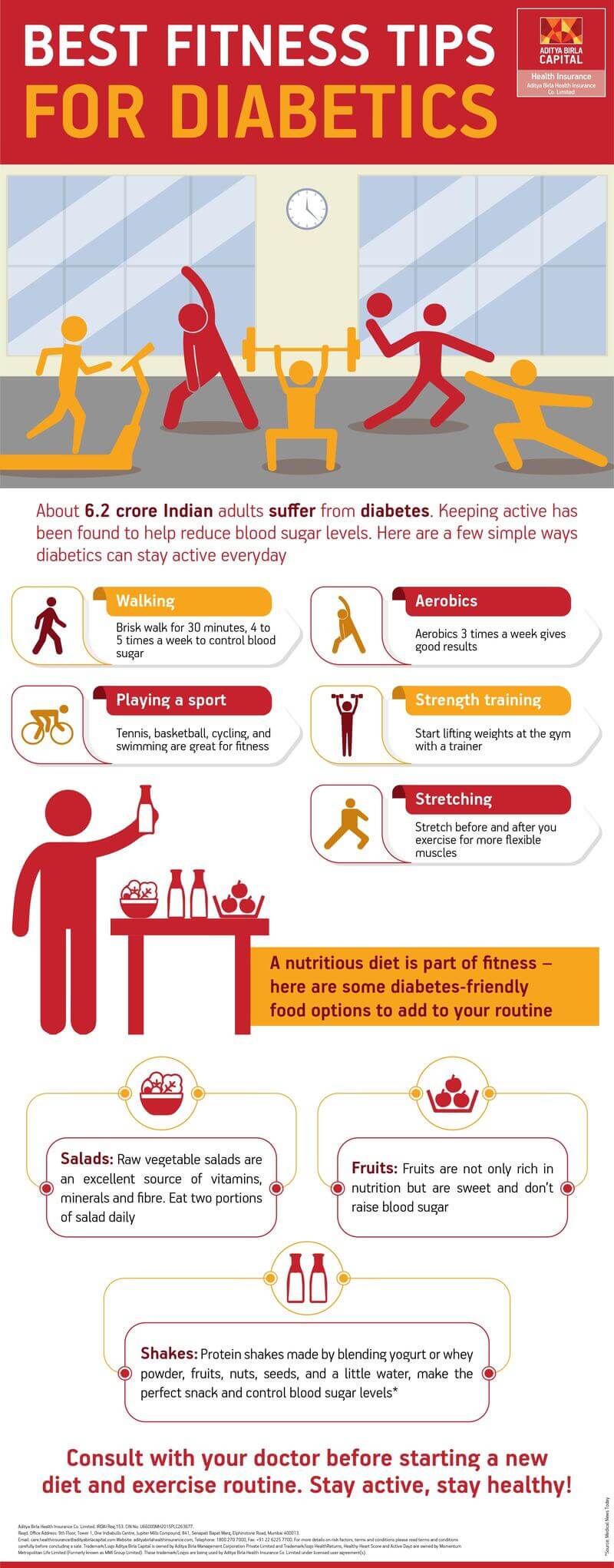
How Regular Physical Activity Impacts Blood Sugar Levels
When we lace up our sneakers and hit the gym, we're not just getting our heart rate up. We're also doing wonders for our blood sugar levels. See, regular physical activity can be one of the most effective ways to help manage and prevent diabetes.
Why is this? Well, when we work out, our bodies need more energy in the form of glucose. So, it taps into our stored glucose reserves (also known as glycogen) to fuel the exercise. This process helps lower high blood sugar levels.
Exercise also makes us more sensitive to insulin - a hormone that plays a crucial role in regulating blood sugar levels. When we're more insulin-sensitive, less of it is required to keep blood sugars at bay. Here are some quick facts:
- Adults should aim for at least 150 minutes of moderate-intensity or 75 minutes of vigorous-intensity aerobic activity per week.
- Strength training exercises should be performed on two or more days each week.
| Activity Type | Duration |
|---|---|
| Moderate-intensity aerobic | At least 150 mins/week |
| Vigorous-intensity aerobic | At least 75 mins/week |
| Strength training | On two or more days each week |
Don't worry if you can't meet these guidelines right away – every little bit helps! Even light activities like walking or gardening can have a positive impact on your blood sugar management.
Remember though: while exercise alone can help control blood sugar levels, it's most effective when combined with other healthy lifestyle habits like eating balanced meals and keeping stress under control.
Creating an Effective Diabetes-Preventive Exercise Plan
Embarking on a journey towards a healthier lifestyle doesn't have to be daunting, especially when it comes to preventing diabetes. A well-structured exercise plan can play a key role in keeping blood sugar levels under control and reducing the risk of type 2 diabetes.
First things first, we recommend starting slow. If you're new to exercising or haven't been active for a while, it's crucial not to overdo it. Aim for about 30 minutes of moderate-intensity activity most days of the week. This could include walking at a brisk pace, swimming or even doing household chores.
Here are some tips that might help:
- Set realistic goals: Don't aim for perfection but strive for consistency.
- Mix up your routine: Including both aerobic exercises like running or cycling, and resistance training such as weight lifting can provide optimum benefits.
- Listen to your body: If you feel pain or discomfort during exercise, take rest and seek professional advice if needed.
Research shows that regular physical activity significantly reduces the risk of developing type 2 diabetes. According to a study published in "Diabetes Care", people who engaged in regular high-intensity exercise had a 40% lower risk of developing diabetes than those who did not participate in such activities.
| Activity Type | Risk Reduction |
|---|---|
| High Intensity Exercise | 40% |
It's also worth mentioning that any amount of physical activity is better than none at all. So don't let the lack of time deter you from staying active. Even short bouts of activity throughout the day can add up and contribute positively towards managing your blood sugar levels.
Adopting an effective diabetes-preventive exercise plan is all about balance - balancing different types of activities, balancing intensity and rest periods, and most importantly balancing exercise with healthy eating habits. Because remember folks - when it comes to preventing diabetes, it's not just about moving more but also eating right.
Conclusion: Turning Exercise Into a Lifelong Habit for Diabetes Prevention
We've delved deep into how exercise can help prevent diabetes. It's clear that physical activity is not just a short-term solution but needs to become a lifelong commitment. Let's wrap up and reinforce some key points.
Regular exercise plays a crucial role in controlling weight, which significantly reduces the risk of developing type 2 diabetes. It's important to remember that consistency trumps intensity when it comes to warding off this disease.
Here are some pointers:
- Aim for at least 30 minutes of moderate-intensity aerobic activity five days a week.
- Incorporate strength training exercises two or more days per week.
- Make your workout routine enjoyable so you'll stick with it long term.
| Type Of Activity | Frequency | Duration |
|---|---|---|
| Aerobic Exercises (like walking, cycling) | At least 5 times per week | Minimum 30 minutes each time |
| Strength Training Exercises (like weight lifting, resistance bands) | At least twice per week | Adjustable as per individual capacity |
Remember, every bit of movement counts. Even activities like gardening or cleaning can contribute to your daily physical activity goal.
But why stop at exercising? Other lifestyle changes can also go hand-in-hand with regular workouts to further reduce your risk of diabetes. Try eating healthily and maintaining an optimal body weight. If you smoke, consider quitting - it's another positive change that could lower your chances of getting diabetes. Ultimately, turning exercise into a lifelong habit won't just prevent diabetes; it will pave the way for better overall health and wellbeing.
References, Studies and Sources:
https://www.cdc.gov/diabetes/managing/active.html
More About Circufiber.com and Healthcare disclaimer:
Always consult your physician before beginning any program. This general information is not intended to diagnose any medical condition or to replace your healthcare professional. If you experience any pain or difficulty, stop and consult your healthcare provider. Circufiber.com socks are clinically proven to improve micro-circulation in feet and lower extremities in people with Diabetes.
More Author Information:
Dr. Capozzi is a board-certified foot surgeon through the American Board of Foot and Ankle Surgery. He is a Diplomate of the American Academy of Wound Management and Fellow of the American College of Foot and Ankle Surgeons. He completed a three-year residency program in Foot and Ankle Reconstructive Surgery at St. Francis Hospital & Medical Center in Hartford, CT in 2010. Dr. Capozzi is a board-certified Wound Specialist® granted by the American Academy of Wound Management. He is also board-certified in Foot Surgery through the American Board of Foot and Ankle Surgery.




