Medically Reviewed by: Scientific Advisory Board
We're diving into a topic that's not often discussed, yet is incredibly important to understand: the distinct difference between diabetes distress and depression. These two conditions may seem similar, but they're far from it. In fact, understanding this distinction can significantly improve the quality of life for those living with diabetes.
Diabetes distress refers specifically to the emotional stress and burden that comes with managing a chronic disease like diabetes. This could range from worry about glucose levels to frustration over diet restrictions. Depression, on the other hand, is a mental health disorder characterized by persistent feelings of sadness or loss of interest in activities once enjoyed.
Recognizing these differences is crucial for ensuring appropriate treatment and support are provided. By clearly differentiating between diabetes distress and depression, we can better tailor our approach to mental health within the diabetes community.
Understanding Diabetes Distress
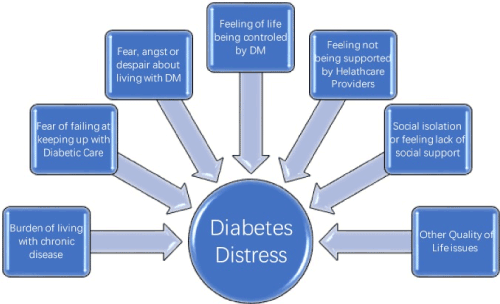
We're diving into the world of diabetes, specifically a psychological aspect known as "diabetes distress". It's an emotional state where people with diabetes feel overwhelmed by the demands and constraints of managing this chronic condition. Frustration, fear, and burnout are common feelings associated with it.
Consider this: you're constantly monitoring your blood sugar levels, counting carbs for every meal, adjusting medication doses, scheduling regular doctor visits - all while trying to live a normal life. That'd be exhausting for anyone. What we've just described is a typical day in the life of someone experiencing diabetes distress.
Let's delve deeper into some numbers here:
| Percentage | Description |
|---|---|
| 18-35% | People with type 1 or type 2 diabetes experiencing significant levels of diabetes distress |
| 45% | Patients who don't discuss emotional problems related to their condition with healthcare providers |
These stats show us that not only is diabetes distress prevalent among those diagnosed but many aren't voicing these struggles to their healthcare professionals.
This silence can lead to detrimental effects on one's overall health and well-being. Not addressing these emotions can result in poor adherence to treatment plans and worse glycemic control. More so, it may escalate to severe mental health disorders such as depression or anxiety.
But here's the silver lining - recognizing and addressing diabetes distress early can significantly improve both mental health outcomes and disease management. So yes, dealing with diabetes can be tough but remember that acknowledging your feelings is a critical step towards better management.
In our upcoming sections, we'll explore more about how you can distinguish between diabetes distress and clinical depression - two conditions often confused due to their overlapping symptoms.
Depression: A Deeper Look
We're diving headfirst into the realm of depression. It's a term that’s tossed around quite casually these days, but it has profound implications. At its core, depression is a serious mental health condition characterized by persistent feelings of sadness and loss of interest in activities once enjoyed.
Depression isn't just "feeling blue". It's an ongoing battle that can cause significant impairment in daily life, making even the most routine tasks feel insurmountable. The National Institute of Mental Health (NIMH) reports that nearly 7% of adults in the U.S experienced at least one major depressive episode in 2017.
| Year | Percentage |
|---|---|
| 2017 | 7% |
Let's understand more about how it presents itself. Symptoms can range from mild to severe and may include:
- Persistent sad or "empty" mood
- Loss of interest or pleasure in hobbies and activities
- Feelings of hopelessness or pessimism
- Irritability
- Decreased energy or fatigue
Though anyone can experience depression, certain factors increase vulnerability such as genetics, brain structure, stress and trauma among others.
Now here's where things get a bit complicated for those with diabetes. Imagine juggling these depressive symptoms on top of managing blood sugar levels, medication schedules and dietary restrictions. This overlap creates what we call 'diabetes distress', which we'll delve into later in this article series.
We must emphasize this - if you're feeling depressed or know someone who might be showing signs, don't hesitate to reach out to healthcare professionals for help. Your mental health matters.
Comparing Symptoms: Diabetes Distress Vs. Depression
In the whirlwind of managing diabetes, it's easy to overlook how our mental health is affected. Two common psychological conditions associated with diabetes are diabetes distress and depression. Although they may seem similar, they're distinct in their nature and require different approaches for management.
Diabetes distress refers specifically to the emotional burden tied to living with and managing diabetes on a daily basis. We're talking about feelings of frustration, worry, or defeat related to the constant monitoring of blood sugar levels, dietary restrictions, medication schedules – the list goes on.
Here are some typical symptoms of diabetes distress:
- Continuous worries about complications
- Concerns over food choices
- Frustration with glucose control
- Fear surrounding hypoglycemia
On the other hand, depression is a more generalized mental health condition that isn't necessarily linked to one’s diabetic condition but can be exacerbated by it. It affects your mood and overall outlook on life.
Symptoms often seen in depression include:
- Persistent feelings of sadness or hopelessness
- Lack of interest in activities once enjoyed
- Difficulty sleeping or oversleeping
- Unexplained physical problems such as back pain or headaches
While there's an overlap in some symptoms between these two conditions like restlessness and irritability, distinguishing them primarily lies in their triggers and scope. With depression being broader than just concerns around diabetes whereas with diabetes distress it's very much focused on managing one’s condition.
It's crucial for us to remember that neither should be taken lightly. If you've noticed any signs pointing towards either condition, don't hesitate to seek professional help because our mental health matters just as much as our physical health when dealing with chronic diseases like diabetes.
Managing Diabetes Distress and Depression
Dealing with diabetes distress and depression can be a challenging feat. We've gathered some essential strategies to help manage these conditions, making the journey a bit more manageable.
Firstly, understanding the difference between these two conditions is pivotal. Diabetes distress refers to the emotional response generated from living with and managing diabetes. It's often associated with feelings of frustration, fear, and burnout related to constant monitoring of blood sugar levels and dietary restrictions. On the other hand, depression is a clinical mood disorder that affects overall happiness and interferes with daily activities.
Recognizing symptoms is crucial in managing both disorders. Some common signs of diabetes distress include:
- Worrying excessively about complications
- Feeling overwhelmed by management regimen
- Frustrating over lack of control over blood glucose
Depression symptoms might involve persistent sadness, loss of interest in activities once enjoyed or changes in appetite or sleep patterns. Keep in mind everyone's experience differs; what may seem like ordinary stress could be an indication of something more serious.
Once we've identified potential signs, it's time to look for solutions. Emotional support plays a significant role here - reaching out to family members or friends can provide relief during difficult times. Joining support groups for individuals dealing with similar challenges can also prove beneficial.
In addition to emotional support, medical intervention might be necessary in some cases. If you're feeling persistently low or anxious, reach out to healthcare professionals who can guide you through appropriate treatment options such as cognitive behavioural therapy (CBT) or medication if required.
It's also worth noting that lifestyle changes can make a significant impact on our mental health status when dealing with diabetes distress and depression:
- Regular physical activity: Exercise releases endorphins known as 'feel-good hormones.'
- Healthy diet: Nutrient-rich food supports overall well-being.
- Adequate sleep: Ensures proper body functioning.
Remember that managing diabetes distress and depression is about finding what works best for you. It's a journey, and it's completely okay to seek help when needed. Always consult with your healthcare provider before making any significant changes to your treatment plan or if symptoms persist.
Conclusion: Emphasizing Mental Health in Diabetic Care
We've come a long way in this piece, unraveling the complexities of diabetes distress and depression. We've seen how both conditions impact the lives of people living with diabetes and emphasized why understanding these differences is crucial for effective care.
Let's underscore one more time that diabetes isn't only a physical burden—it also presents significant mental health challenges. Clear distinctions between diabetes distress and depression are necessary to ensure we're directing our efforts effectively when providing support.
Remember, it's not just about managing blood sugar levels but also about taking care of your mental well-being. People with diabetes who experience feelings of distress or symptoms of depression should seek help from healthcare professionals trained to address these issues.
Here are some key takeaways from our discussion:
- Diabetes distress arises primarily due to the daily demands and pressures associated with managing the disease.
- Depression in individuals with diabetes may be linked to various factors—not exclusively related to their condition—and requires professional diagnosis.
- Treating both conditions may involve different approaches, emphasizing the need for personalized patient care plans.
We hope this piece has shed light on your understanding of these two distinct yet interconnected aspects of diabetic care. Remember, you're not alone—seek out support when you need it, communicate openly with your healthcare team, and prioritize self-care alongside disease management.
Finally, let's remember that awareness is half the battle won. By acknowledging the importance of mental health within diabetic care, we can create better strategies for managing not only the physical symptoms but also enhancing overall quality of life for those grappling with this challenging condition. May our exploration serve as a stepping stone towards broader discussions and innovations in diabetic mental health care.
Research, Resources, Studies:
https://www.diabetes.org.uk/guide-to-diabetes/emotions/diabetes-burnout
More About Circufiber.com and Healthcare disclaimer:
Always consult your physician before beginning any program. This general information is not intended to diagnose any medical condition or to replace your healthcare professional. If you experience any pain or difficulty, stop and consult your healthcare provider. Circufiber.com socks are clinically proven to improve micro-circulation in feet and lower extremities in people with Diabetes.
More Author Information:
Dr. Capozzi is a board-certified foot surgeon through the American Board of Foot and Ankle Surgery. He is a Diplomate of the American Academy of Wound Management and Fellow of the American College of Foot and Ankle Surgeons. He completed a three-year residency program in Foot and Ankle Reconstructive Surgery at St. Francis Hospital & Medical Center in Hartford, CT in 2010. Dr. Capozzi is a board-certified Wound Specialist® granted by the American Academy of Wound Management. He is also board-certified in Foot Surgery through the American Board of Foot and Ankle Surgery.




