Medically Reviewed by: Scientific Advisory Board
When discussing diabetic feet pictures in the beginning stages, we want to help our readers understand the early signs and symptoms of diabetic foot complications. Diabetic foot problems can become quite serious if left untreated, so it's essential to be proactive in identifying and addressing any issues early on. By being aware of the initial changes in your feet and seeking appropriate medical care, you can potentially prevent more advanced complications and maintain your overall health.

Diabetic feet problems often begin with subtle changes that can be easy to miss if you're not paying close attention to your feet. Some initial indicators may include persistent redness, swelling, and increased warmth in the affected area. Wounds or ulcers that appear small at first but don't seem to be healing could also signal the start of a developing issue. Additionally, changes in skin color or texture, such as dry or scaly skin, may be early warning signs.
To better recognize and understand the initial stages of diabetic foot complications, we'll delve into various factors that contribute to the development of these issues, the importance of proper foot care, and the role healthcare professionals play in diagnosis and treatment. Through examining these images and providing guidance, our aim is to help those with diabetes take the necessary steps to prevent foot problems and enjoy a healthier future.
Understanding Diabetic Feet
Diabetic feet issues are a common concern for people with diabetes. They stem from a combination of factors, including nerve damage, poor circulation, and infection. Early detection and treatment are crucial to minimize the risk of severe complications. In this section, we'll delve into the beginning stages of diabetic foot problems and provide insight into their progression.
Nerve damage, or neuropathy, is a major contributing factor to diabetic feet. Over time, high blood sugar levels can damage nerves, causing numbness and reduced sensation in the feet. This means it's harder for us to feel an injury or irritation, which can go unnoticed and develop into a more serious issue. Some common symptoms of neuropathy include:
- Tingling sensation
- Burning or sharp pains
- Loss of sensation
- Muscle weakness
Poor circulation is another significant factor. Diabetes can affect blood flow by narrowing the blood vessels in the legs and feet, making it difficult for oxygen and nutrients to reach the affected areas. This impairs the body's ability to heal and ups the chances of infections. Signs of poor circulation include:
- Cold feet
- Slow healing sores or ulcers
- Changes in skin color
- Swelling or pain in the legs
When it comes to infection, high blood sugar levels can weaken the immune system, making it harder for our bodies to fight off infections. When an injury or even a minor cut occurs, bacteria can enter the wound, leading to infection. If left untreated, the infection can escalate, potentially leading to severe complications, including amputation.
In the beginning stages of diabetic foot problems, preventative measures can be very effective. Here are a few steps we can take to help safeguard our feet:
- Regular self-examination
- Proper foot hygiene
- Wearing comfortable, well-fitted shoes
- Using moisture-wicking socks, like those from Circufiber.com
- Managing blood sugar levels
By staying well-informed and actively working to prevent diabetic foot issues, we stand a better chance at maintaining our foot health and staying ahead of complications. Keep an eye out for any changes in appearance, sensations, or unexpected wounds in the feet - they might be signaling the onset of more significant issues. Seeking prompt medical attention and employing good foot care practices can make all the difference in the early stages of diabetic feet problems.
Early Symptoms to Watch For & Diabetic Feet Pictures
Diabetic foot complications can progress rapidly, so identifying early symptoms is crucial for successful treatment and management. In this section, we'll discuss some of the initial signs to be aware of:
-
Tingling or numbness: One of the first indicators of potential diabetic foot problems is a tingling sensation or numbness in your feet. This might signify nerve damage or neuropathy, a common issue among people with diabetes.
-
Increased sensitivity to touch: You may notice that your feet are more sensitive to touch than before. This is another sign of neuropathy, and it's essential to monitor this symptom closely.
-
Pain or cramping: Experiencing pain or cramping in your legs or feet may indicate circulatory issues or nerve damage, which are common complications in diabetics.
-
Changes in skin color or temperature: Pay attention to any changes in your feet's skin color or if they feel unusually hot or cold to the touch. This could signal poor circulation or the beginning of an ulcer.
-
Dry skin: Dry, cracked skin on your feet might be a sign of nerve damage or poor circulation, both of which are risk factors for foot ulcers and infections.
-
Cuts, blisters, or sores that do not heal: If you notice that any cuts, blisters, or sores are taking longer to heal than usual, this may be due to poor blood flow or your body's impaired ability to heal itself.
To further illustrate the most common initial signs of diabetic foot issues, we've created the table below:
| Symptom | Possible Cause |
|---|---|
| Tingling or numbness | Nerve damage or neuropathy |
| Increased sensitivity to touch | Neuropathy |
| Pain or cramping | Circulatory issues or nerve damage |
| Changes in skin color or temperature | Poor circulation or early ulcer formation |
| Dry skin | Nerve damage or poor circulation |
| Cuts, blisters, or sores that do not heal | Poor blood flow or impaired healing |
It's vital to address these early symptoms before they evolve into more severe complications. As a diabetic, you should regularly inspect your feet for any of these signs, and if you notice them, consult your healthcare provider immediately.
We hope this information aids you in identifying the early symptoms of diabetic feet problems so you can better manage your diabetes health. Stay vigilant, and remember to take care of your feet.
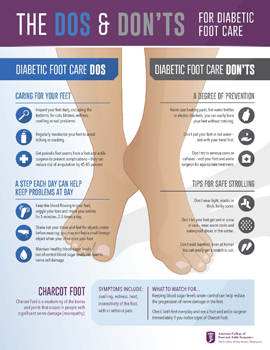
How to Protect Your Feet
Taking preventative measures to protect your feet is crucial when you have diabetes. Following these tips can help reduce the risk of complications and ensure that your feet stay healthy.
Regular Inspections: Check your feet daily for any cuts, blisters, sores, or infections. If you notice any changes, consult a healthcare professional immediately.
Proper Footwear: Opt for well-fitting, comfortable shoes that provide adequate support and cushioning. Avoid tight shoes, high heels, or shoes with thin soles.
Moisturize and Dry: Keep your feet moisturized by applying lotion or cream to avoid dry, cracked skin. At the same time, dry your feet thoroughly after bathing or swimming, particularly between the toes.
Toe and Nail Care: Trim your toenails regularly and file any sharp edges. Don't trim too short, as this can lead to ingrown toenails. Wear breathable, moisture-wicking socks to minimize the risk of fungal infections.
Daily Exercise: Engage in regular physical activity to improve blood circulation in your feet. Talk to your healthcare provider to determine an appropriate exercise regimen for you.
Avoid Extreme Temperatures: Protect your feet from extreme heat or cold. Wear appropriate footwear and avoid walking barefoot.
Quit Smoking: Smoking narrows and hardens your arteries, limiting blood flow and increasing your risk of foot-related complications.
Control Blood Sugar: Maintain your blood sugar within your target range to minimize the impact of diabetes on your foot health.
Regular Podiatrist Visits: Schedule regular appointments with a podiatrist to monitor your foot health and address any potential issues early on.
Incorporating these practices into your daily routine can significantly reduce the risk of diabetic feet complications. Remember to always stay vigilant and consult with healthcare professionals when necessary. Ultimately, proactive care is the key to protecting your feet and enjoying a healthier, happier lifestyle with diabetes.
What to Do Next: A Conclusion
It's essential to address any signs of diabetic foot issues promptly to prevent complications. Taking action early can help protect your feet and maintain overall health. In this conclusion, we'll walk through some key steps to take if you suspect problems with your diabetic feet.
Firstly, consult a healthcare professional. Whether it's a general practitioner, a podiatrist, or an endocrinologist, getting expert help is crucial. Explain your concerns, share any pictures or symptoms you've noticed, and collaborate on a plan of action. Remember that early intervention is the best way to avoid more serious complications.
Next, invest in proper foot care. This means:
- Keeping your feet clean and dry
- Moisturizing to prevent dry, cracked skin
- Trimming your toenails properly
- Wearing well-fitted shoes
- Avoiding walking barefoot
- Inspecting your feet daily for any changes
Maintaining good blood sugar levels is another essential aspect of diabetic foot care. Work with your healthcare provider to develop a personalized plan to control your blood glucose, track progress, and adjust medications if needed.
We hope this article has provided valuable insights on the beginning stages of diabetic feet issues and the importance of taking action right away. By following these steps, our goal is to empower you to keep your feet healthy and avoid complications. Remember, it's never too early to start taking care of your feet. Always stay proactive and seek advice from trusted medical professionals.
References, Studies and Sources:
https://www.cdc.gov/diabetes/library/features/healthy-feet.html
https://my.clevelandclinic.org/health/diseases/21510-diabetic-feet
More About Circufiber.com and Healthcare disclaimer:
Always consult your physician before beginning any program. This general information is not intended to diagnose any medical condition or to replace your healthcare professional. If you experience any pain or difficulty, stop and consult your healthcare provider. Circufiber.com socks are clinically proven to improve micro-circulation in feet and lower extremities in people with Diabetes.
More Author Information:
Dr. Capozzi is a board-certified foot surgeon through the American Board of Foot and Ankle Surgery. He is a Diplomate of the American Academy of Wound Management and Fellow of the American College of Foot and Ankle Surgeons. He completed a three-year residency program in Foot and Ankle Reconstructive Surgery at St. Francis Hospital & Medical Center in Hartford, CT in 2010. Dr. Capozzi is a board-certified Wound Specialist® granted by the American Academy of Wound Management. He is also board-certified in Foot Surgery through the American Board of Foot and Ankle Surgery.